
Write something
What if hunger isn’t the enemy… (the small frequent meal myth)
What if hunger isn’t the enemy, but one of your body’s most powerful metabolic signals? For decades we were told to eat constantly. “Six small meals a day.” “Never skip breakfast.” “Keep the metabolism firing.” But biologically, the human body was never designed to be in a constant fed state. For most of human history, periods of eating and periods of fasting naturally alternated. And those fasting windows triggered some of the most important repair processes in the body. When we constantly digest food, the body prioritizes storage and growth. When we pause from eating, the body shifts toward repair and restoration. This metabolic transition is sometimes called “the metabolic switch.” Instead of relying primarily on glucose for fuel, the body begins shifting toward fat oxidation and ketone production. And that shift activates several powerful biological processes. 1️⃣ Cellular Cleanup (Autophagy) Fasting helps trigger autophagy, the cellular recycling system that removes damaged proteins, dysfunctional mitochondria, and metabolic debris. This process was so important that it earned the 2016 Nobel Prize in Physiology or Medicine. Autophagy supports: • mitochondrial health • cellular repair • metabolic resilience 2️⃣ Metabolic Flexibility Many people today are metabolically inflexible — meaning their bodies rely almost exclusively on glucose for energy. Periods of fasting help restore the body’s ability to switch between fuel sources: glucose → fat → ketones This metabolic flexibility is associated with: • improved insulin sensitivity • more stable energy • better appetite regulation 3️⃣ Hormonal Recalibration Hunger is largely regulated by two hormones: Ghrelin — signals hunger Leptin — signals satiety Constant eating disrupts these signals. Strategic fasting can help restore normal hunger and fullness cues, allowing people to experience what true hunger — and true satiety — actually feel like again. But fasting is not one-size-fits-all.

What Is “Leaky Gut”? (Part 2)
Understanding Intestinal Permeability and How We Restore the Gut Lining One of the most important concepts in functional and root-cause medicine is something called intestinal permeability—often referred to as “leaky gut.” Despite the nickname, this isn’t a trendy wellness buzzword. It’s a well-documented physiological process that plays a central role in inflammation, immune dysfunction, metabolic disease, and many chronic symptoms. To understand why, we need to understand what the intestinal barrier is actually designed to do. The Gut Lining: Your Body’s Most Important Security Gate Your intestinal lining is only one cell thick, yet it covers about 4,000 square feet of surface area—roughly the size of a tennis court. Its job is incredibly precise. It must allow nutrients to pass through, while blocking: • toxins • pathogens • undigested food particles • inflammatory molecules Think of it like a security checkpoint at the airport. The gut lining uses microscopic structures called tight junctions to regulate what enters the bloodstream. When those junctions are working properly, the barrier is selectively permeable—nutrients get through, harmful substances stay out. But when the lining becomes damaged or inflamed, those tight junctions loosen. And that’s where problems begin. What Happens When the Gut Becomes “Leaky” When intestinal permeability develops, the gut barrier stops functioning like a smart filter and begins acting more like a sieve. Substances that should never enter circulation begin leaking into the bloodstream, including: • bacterial toxins (LPS endotoxin) • partially digested proteins • inflammatory compounds • microbial fragments When these particles cross into the bloodstream, the immune system treats them like invaders. This triggers chronic low-grade inflammation, which can manifest as: • food sensitivities • skin issues (eczema, acne, psoriasis) • brain fog • fatigue • joint pain • autoimmune conditions • metabolic dysfunction
1
0

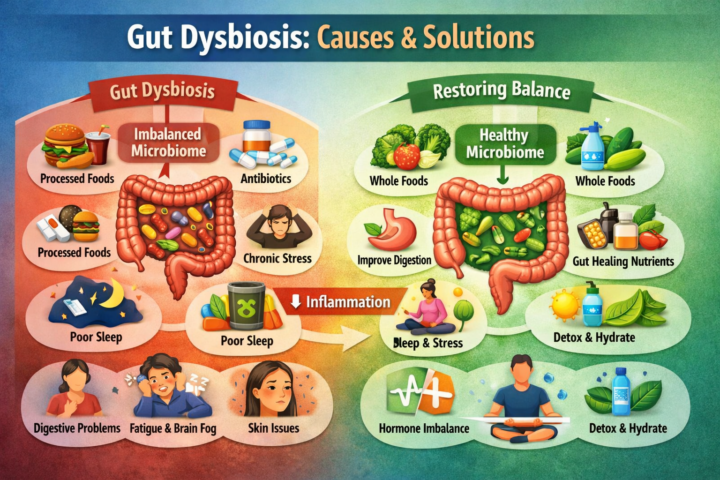
Gut Dysbiosis: What It Is, What Causes It, and How We Restore Balance (Part 1)
One of the most common root causes behind chronic health issues is something many people have never heard of: gut dysbiosis. Dysbiosis simply means an imbalance in the microbiome—the ecosystem of bacteria, fungi, and other microbes living in your digestive tract. A healthy gut isn’t sterile. It’s diverse, balanced, and resilient. Your microbiome helps regulate: • digestion • nutrient absorption • immune function • inflammation • hormones • brain chemistry • metabolism In fact, 70–80% of your immune system lives in the gut, and your microbiome produces many of the neurotransmitters that influence mood, sleep, and cognition. When this ecosystem becomes imbalanced, symptoms can start showing up almost anywhere in the body. What Gut Dysbiosis Looks Like Many people assume gut problems only show up as digestive symptoms. Sometimes they do, but not always. Common digestive signs: • bloating • gas • constipation or diarrhea • reflux • food sensitivities • abdominal pain But dysbiosis also shows up in ways that seem unrelated to the gut: • fatigue • brain fog • anxiety or depression • skin issues (eczema, acne, rosacea) • joint pain • autoimmune conditions • weight gain or metabolic dysfunction • hormone imbalance • poor immune resilience This happens because the gut acts as a control center for inflammation and immune signaling throughout the body. When the microbiome is out of balance, the entire system becomes dysregulated. What Causes Gut Dysbiosis Dysbiosis rarely happens from one thing. It’s usually the result of multiple pressures on the microbiome over time. The most common drivers include: 1. Ultra-processed foods Highly processed foods are typically low in fiber and high in refined carbohydrates, seed oils, preservatives, and emulsifiers. These ingredients feed opportunistic bacteria while starving beneficial microbes. 2. Antibiotics Antibiotics can be lifesaving when necessary, but they also wipe out beneficial bacteria. Many people never fully rebuild their microbiome afterward.
2
0
Why “Eating Less” Doesn’t Lead to Weight Loss:
Calories in/ Calories out is a MYTH Eating less and exercising more is NOT the recipe for healthy sustainable weight loss. One of the most common frustrations I hear from clients is this: “I’m eating less… but the scale won’t move.” And in many cases, they’re telling the truth. Because weight loss is not just a calorie equation. It’s a metabolic regulation problem. In clinical practice, we frequently see plateaus that occur not because someone lacks discipline — but because the body is responding to physiological stress signals. Here are some of the most common mechanisms behind it. ⸻ 1️⃣ Metabolic Adaptation When calories drop aggressively, the body activates a survival response. Research shows Basal Metabolic Rate (BMR) can drop 10–15% or more during prolonged calorie restriction. The body simply burns fewer calories to conserve energy. This is why chronic dieting often leads to plateaus or rebound weight gain. ⸻ 2️⃣ Insulin Resistance Insulin acts as the gatekeeper for energy storage and release. When insulin levels remain elevated: • fat burning is suppressed • fat storage is promoted • energy becomes trapped in fat cells This is one reason abdominal fat can increase even when calorie intake is reduced. ⸻ 3️⃣ Chronic Stress & Cortisol This is the piece many people underestimate. Poor sleep, work stress, and nervous system overload keep cortisol elevated. Cortisol increases: • blood sugar • insulin signaling • visceral fat storage • inflammatory signaling In other words: The body shifts toward energy storage instead of energy burning. ⸻ 4️⃣ The Gut–Metabolic Axis Your microbiome plays a major role in metabolic regulation. Gut dysbiosis has been strongly linked to: • insulin resistance • chronic inflammation • impaired nutrient signaling • altered energy extraction from food In other words, the gut influences how the body interprets food metabolically. ⸻ The Real Shift in Approach Weight loss is rarely just about eating less.
3
0

🪨 Back to Bedrock: 7 Health Narratives That Deserve a Second Look
One of the core principles we teach inside Bedrock is this: Human biology hasn’t changed in 100,000 years. What’s changed is our environment, food system, and messaging. Most people are not “failing” at health. They are following advice that was never designed around human physiology. Below are 7 common health narratives worth examining more closely—not as dogma, but through the lens of terrain, context, and biology. 1️⃣ “Fat makes you fat” Fat is not just fuel—it’s structural. • Cell membranes are lipid-based • Hormones are synthesized from fat • The brain is ~60% fat When dietary fat was removed, it was replaced with refined carbohydrates and industrial seed oils. That shift correlated with rising insulin resistance, inflammation, and metabolic dysfunction—not improved health. Takeaway: The issue isn’t fat. It’s metabolic context. 2️⃣ “Red meat causes cancer” Most studies do not distinguish between: • Grass-fed, whole cuts of meat • Ultra-processed meats with preservatives and fillers Humans consumed animal protein long before modern chronic disease became widespread. Takeaway: Processing matters more than the food itself. 3️⃣ “Sunlight is dangerous” Sun exposure regulates: • Vitamin D synthesis • Immune function • Circadian rhythm • Mood and hormone signaling Avoidance without context can contribute to deficiency and dysregulation. Takeaway: Intelligent exposure > total avoidance. 4️⃣ “Breakfast is the most important meal” This idea emerged alongside packaged food marketing. Historically, humans ate when food was available—not by the clock. Constant eating keeps insulin elevated and limits metabolic flexibility. Takeaway: Timing should support your physiology, not a slogan. 5️⃣ “Cholesterol is the enemy” Cholesterol is essential for: • Hormone production • Brain and nerve function • Cell repair Cardiovascular risk correlates more strongly with inflammation, insulin resistance, and metabolic health than cholesterol alone. Takeaway: Markers matter—but so does context.

1-26 of 26
powered by

skool.com/bedrock-nation-8489
Free wellness community for faith based living, functional health and real connection - off social media, rooted in purpose - learn, grow and heal.
Suggested communities
Powered by
