Activity
Mon
Wed
Fri
Sun
Jun
Jul
Aug
Sep
Oct
Nov
Dec
Jan
Feb
Mar
Apr
May
What is this?
Less
More
Owned by Ellen
Mentoring women to master everyday homeopathy for natural, confident care for themselves and their families.
Memberships
Roots Of England
62 members • Free
Vagus School
789 members • Free
🇺🇸 Atlanta IRL
193 members • Free
AI Automation Society
364.9k members • Free
The Cyber Community
8.6k members • Free
Making Better Agents
628 members • Free
AI Cyber Value Creators
8.8k members • Free
Skoolers
188.9k members • Free
The Transurfing Skool
3.9k members • Free
5 contributions to Vagus School
The Octopus and the Question of Where Intelligence Lives
Part 1 of a three-part series on distributed biological intelligence. Octopuses have become something of a celebrity in popular neuroscience, and it's easy to see why. They open jars, they recognize individual humans, they squeeze their soft bodies through implausibly small holes, and they do all this with a nervous system that looks nothing like ours. The detail that gets repeated most often is that an octopus has roughly 500 million neurons, but only a small fraction of them are in the head. Most are spread out through the eight arms. That number is real. The central brain is estimated at around 40 to 50 million neurons. The paired optic lobes add something like 130 million on top of that. And the eight arms together house around 350 million — somewhere in the neighborhood of two-thirds of the entire nervous system. Connecting all of it is a surprisingly thin wire: by classic estimates, only about 30,000 nerve fibers run between the central brain and the arm cords. If you're used to the idea that intelligence happens in a brain, full stop, this picture is genuinely disorienting. Where is the octopus actually thinking? The honest answer is that we don't fully know. But we know enough to say that the octopus arm is doing real work. Each arm contains a thick axial nerve cord running its full length, four smaller intramuscular nerve cords alongside it, and a small ganglion at the base of every single sucker. There can be hundreds of suckers per arm. Recent imaging has sharpened the picture considerably. Olson, Schulz and Ragsdale published a striking 2025 paper in Nature Communications showing that the axial nerve cord isn't a uniform tube but is organized into segments, with cell bodies arranged in repeating columns and a topographic map of the suckers built right into the wiring. A 3D molecular atlas published the year before by Winters-Bostwick and colleagues in Current Biology added another layer of detail, identifying multiple distinct neurochemical cell types whose distribution differs from arm base to arm tip.

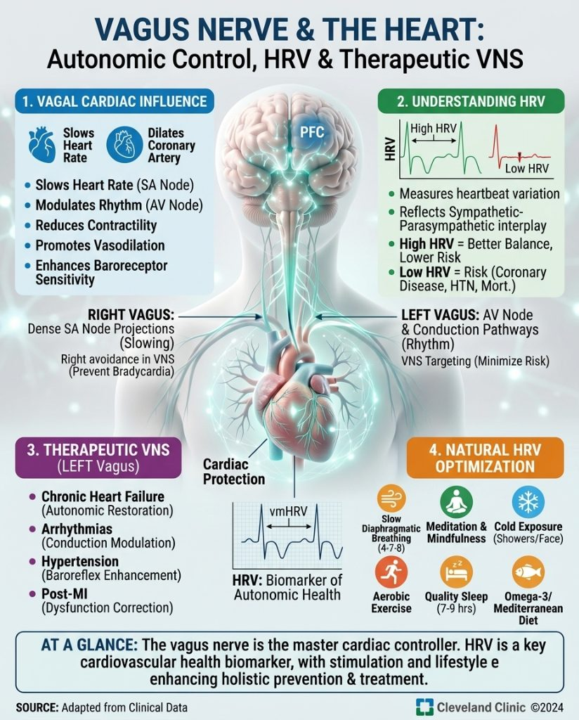
Using HRV Monitoring To Unlock Your Vagus Nerve For A Healthier Heart
The vagus nerve is the main parasympathetic nerve to the heart, providing rest and digest counterbalance to sympathetic fight or flight signals. Vagal stimulation slows heart rate, reduces contractile force, and promotes coronary artery dilation. The right vagus nerve has denser cardiac projections than the left, explaining avoidance of right-sided stimulation in VNS to prevent bradycardia or transient asystole. Through cardiac branches, the vagus nerve influences heart rate by slowing the sinoatrial node, rhythm by modulating atrioventricular node conduction, contractility by reducing force during rest, coronary blood flow by dilating arteries, baroreceptor sensitivity for blood pressure responses to position changes, and heart rate variability. Heart rate variability (HRV) measures variation in time between consecutive heartbeats. Higher HRV reflects dynamic sympathetic-parasympathetic interplay, stronger vagal tone, better autonomic balance, improved cardiovascular health, lower stress, and reduced mortality risk. Low HRV indicates vagal withdrawal and sympathetic dominance, linked to increased risk of coronary artery disease, heart attacks, sudden cardiac death, heart failure progression, hypertension, type 2 diabetes, all-cause mortality, chronic stress, burnout, anxiety, depression, poor physical fitness, inflammation, aging, and reduced longevity. Vagus nerve stimulation (VNS) targets cardiovascular conditions. In chronic heart failure, VNS restores autonomic balance, potentially improving cardiac function, exercise tolerance, and quality of life; early trials show promise as adjunctive therapy. For arrhythmia management, VNS modulates electrical conduction, relevant for atrial fibrillation and supraventricular arrhythmias, potentially reducing episodes or enhancing treatment outcomes. In hypertension, VNS enhances baroreflex sensitivity for blood pressure regulation during postural changes and stress, offering benefits for resistant cases. Post-myocardial infarction, VNS addresses persistent autonomic dysfunction to improve long-term outcomes and prevent recurrence. In coronary artery disease, vagal stimulation promotes vasodilation, improves endothelial function, and may reduce atherosclerotic progression.
Used Ultrasound on Belly; I Feel Really Good. ☺️
I got it in my head to try my US 2000 ultrasound device on my belly. Call it intuition, a download, scientific curiosity, whatever you want. Being the mad scientist biohacker that I am, I went with it. It's been about 20 minutes since I finished, and I feel pretty darn good, emotionally. I suffer from depression, so a feeling this good really stands out. If my mood started at a 3, it is now an 8. What's interesting is that the positive feelings didn't start immediately after the treatment. They slowly built over the next 15-20 minutes. I didn't even notice until I realized, "Hey, I feel pretty good." I've experimented using the ultrasound on my vagus nerve and forehead, but didn't experience any emotional effect, nor was I expecting it. This alleged positive effect using it on my belly was a surprise. I went into it completely open-minded. I'm going to continue experimenting to make sure it's not placebo and to see it's limits. I just wanted to share this with my fellow mad scientists if you wanted to experiment as well. Good day! Rob
Tinnitus Relief: Tapping The Vagus Nerve For A Quieter Life
Tinnitus: a relentless phantom sound impacting millions. The source? Disrupted neuroplasticity in auditory pathways. A promising solution: targeted vagus nerve stimulation (tVNS). tVNS paired with pure sine wave tones, calibrated to individual tinnitus frequencies. Vagus nerve stimulation activates anti-inflammatory pathways. Norepinephrine and acetylcholine flood the brain, amplifying synaptic plasticity. Precise VNS pulses during tone exposure create Hebbian-like strengthening. This reprograms sensory maps, similar to phantom limb pain therapies. Early results: reduced ringing intensity and improved focus. A scalable, non-invasive path to relief. Explore protocols and share progress in the Vagus Skool Group Here: https://www.skool.com/vagus/tinnitus

Welcome to Vagus Skool ! (Start Here) ✊
This is a Free to Join Skool Community! A community designed to help people Stimulate and Repair their Vagus Nerve! Comment Below! - What you know about the Vagus Nerve 🦄 - Your preferred method of Vagus Nerve Stimulation ? (Breath, TENS, Ultrasound, etc?) 👩💼 - A Want or Have Had Experience from Vagus Nerve Land !? (A win, or something you are striving for) And when you comment, like a post, get 5 likes across your comments, and click "Complete" on a few of the modules in the Classroom, you can then unlock the Ultrasound module ! YAY ! So, I hope this can become a great community page, it's very open, and you have access to SO MUCH good information, actionable information, on the Vagus Nerve, and all the ways you can make it happy and healthy ! So from the Vagus Skool to you and yours... WELCOME !

1-5 of 5
@ellen
Southern gal, former ER PA (20+ yrs), Ed.D. in biology, now integrative homeopath passionate about women’s wellness & natural healing.
Active 4h ago
Joined Mar 13, 2026
Atlanta, GA
Powered by



