Activity
Mon
Wed
Fri
Sun
Jul
Aug
Sep
Oct
Nov
Dec
Jan
Feb
Mar
Apr
May
What is this?
Less
More
Owned by Dementia
Dementia Care Support & Expert Guidance.
Memberships
198 contributions to The Dementia Lifeboat
Jocelyn's Thursday Thought
The happiest people I know do this one thing consistently and on purpose. They get excited about all the little things. The perfect cup of coffee in the morning. Finding a great new song to add to their playlist. The show they are watching. Seeing their kid's name pop up on their phone. A new pair of earrings. A walk on a cool day. Their pet's sweet little face. A sale at their favorite store. Clean sheet night. Rain. They don't wait for life to get better or bigger to feel happy and alive. They decide this one is worthy of their love. That's the difference. I know there is a resistance to loving your life just as it is because most think it will stop them from trying to make it better. But, they simply have it backwards. Because you are 100% allowed to love this life and strive for a better one. In fact, loving all the good you have right now creates the very emotions needed to make any changes that you desire. Be more in love with your everyday life and watch your whole life change. Ironically enough, the quickest way to your version of big happy is to slow down and collect little "happys" all along the way. What are you waiting for? Find your happy. Have a beautiful week! I love you all, Jocelyn
0
0
When should we host our discussions?
We want to hear from YOU! What days and times work best for you to meet up to have an open conversation with Laura, Jocelyn, and your peers? Please drop suggestions in the comment box below!
Poll
1 member has voted
Thank You For Joining! 💜
Thank you to everyone who attended the Poolside Chat last night! If you missed our conversation, you can watch the recording here: https://www.skool.com/dementia-lifeboat/classroom
0
0
Join Us Tonight!
Join us live this evening at 5:30 PM Arizona time: https://us02web.zoom.us/meeting/register/PRzPtXKIRf-NNdHzhSToUg#/registration
0
0

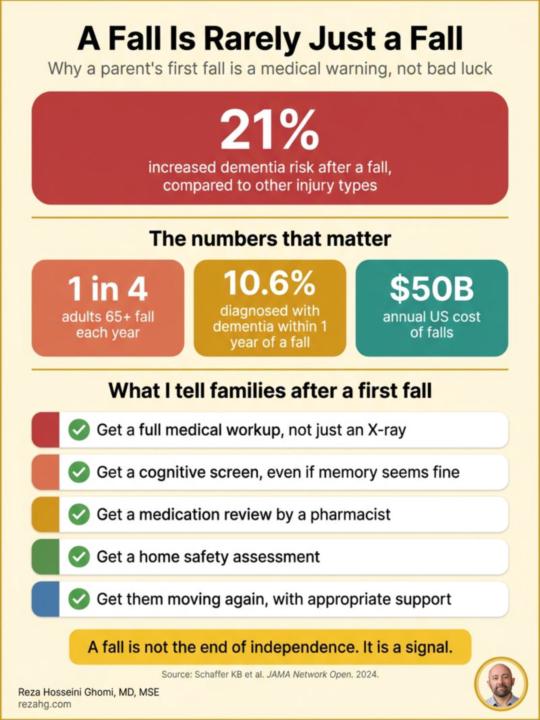
A Fall Is Rarely Just A Fall
After 15 years of seeing this in clinic, I have learned to treat a fall in an older adult as a warning shot. Not as bad luck. Not as carelessness. A signal that something has changed. Here is what the data shows. 1. Falls are the leading cause of injury in older adults ↳ 1 in 4 adults over 65 falls each year ↳ Falls cause 3 million ER visits annually ↳ Costs the system about $50 billion a year 2. A fall predicts cognitive decline ↳ A 2024 JAMA study of 2.4 million older adults found that 10.6% of those who fell were diagnosed with dementia within 1 year ↳ Falls were associated with a 21% increased dementia risk compared to other injury types ↳ A fall should trigger cognitive screening. Most of the time, it does not. (The authors address fall -> dementia vs. dementia -> fall) 3. The cascade after a first fall is brutal ↳ Fear of falling reduces activity ↳ Reduced activity worsens strength and balance ↳ Worse strength leads to more falls ↳ More falls lead to fractures, hospitalizations, and decline 4. The risk factors are mostly addressable ↳ Vision and hearing problems ↳ Medications that affect balance or blood pressure ↳ Untreated sleep disorders ↳ Loss of muscle mass and strength ↳ Home hazards ↳ Vitamin D deficiency ↳ Postural blood pressure changes 5. The best interventions are not the obvious ones ↳ Strength training, not just balance exercises ↳ Reviewing medications, not just adding grab bars ↳ Treating hearing loss, not just removing throw rugs ↳ Addressing the underlying cause, not just the symptom What I tell families when someone they love has fallen for the first time. Get a full medical workup. Not just a knee X-ray. Get a cognitive screen, even if no one thinks it's needed. Get a medication review by a pharmacist. Get a home safety assessment. Get them moving again, with appropriate support. A fall is not the end of independence. It is a signal that the system needs attention. If you are a family member who has noticed your parent slowing down, do not wait for the fall to do something about it.
0
0
1-10 of 198
Active 2d ago
Joined Dec 18, 2024
United States
Powered by

